Sciatica: Causes, Symptoms & How Spinal Decompression Offers Relief
Sciatica is one of the most common types of pain associated with the lower back, affecting millions of people worldwide. It’s not a disease in itself, but a symptom of underlying nerve irritation or compression, usually involving the sciatic nerve — the longest and widest nerve in the body. Sciatic pain can range from mild discomfort to debilitating pain that radiates from the lower back down the leg, making everyday activities difficult or impossible.
In this article, we’ll explore what sciatica is, how it develops, its symptoms, its impact on everyday life, conventional treatment approaches, and how spinal decompression therapy — especially as offered by The Decompression Clinic — provides a non-surgical, drug-free option for many people suffering from sciatica.
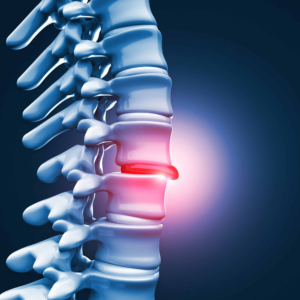
What Is Sciatica?
Sciatica refers to pain along the path of the sciatic nerve, which originates from the lower spine and travels through the buttocks and down the back of each leg. It is caused by nerve compression or irritation, usually in the lumbar spine, that affects the nerve roots feeding into the sciatic nerve.
Rather than being a disease, sciatica describes a set of symptoms that indicate nerve dysfunction. Pain typically travels from the lower back or buttock and radiates down one leg — sometimes all the way to the foot — following the pathway of the nerve.
The pain is often described as sharp, electric, burning, or “shooting” and tends to worsen with certain movements, like bending forward, coughing, or prolonged sitting.
Anatomy of the Sciatic Nerve
The sciatic nerve is formed by nerve roots from the lower lumbar and sacral spine — typically L4, L5, S1, S2, and S3 — which converge in the pelvis and extend down each leg. It controls the muscles of the back of the knee and lower leg and provides sensation to much of the lower limb.
Because of its size and distribution, compression or irritation anywhere along this long nerve can result in widespread symptoms that affect mobility, sensation, and comfort.
What Causes Sciatica?
Sciatica usually occurs because the sciatic nerve — or one of its nerve roots — is pinched or irritated. The most common underlying causes include:
01.
Herniated or Bulging Discs
A disc in the lumbar spine can bulge or rupture and press on nearby nerve roots, triggering sciatica. This is the most frequent cause of sciatica pain, especially in adults under 50.
02.
Bone Spurs and Spinal Stenosis
As people age, degenerative changes like bone spur formation or narrowing of the spinal canal (spinal stenosis) can compress nerves. This is a common cause in older adults.
03.
Spondylolisthesis
When one vertebra slips forward over another, it can compress nerve roots.
04.
Piriformis Syndrome & Soft Tissue Irritation
In some cases, tight muscles — such as the piriformis in the buttocks — can irritate the sciatic nerve as it passes underneath, producing similar symptoms.
05.
Trauma or Injury
Direct injury to the lower back or pelvis can lead to nerve damage or compression.
06.
Other Nerve Compression Conditions
Nerve compression from infection, tumors, or rarer causes like epidural hematoma can produce sciatica-like symptoms, though these are less common.
- FOR ASSISTANCE
Symptoms of Sciatica
The hallmark of sciatica is radiating pain — typically one-sided — that follows the path of the sciatic nerve down the leg. Yet the condition may produce a variety of symptoms, including:
- Sharp, burning or electric pain in the lower back, buttock, or leg.
- Tingling or “pins and needles” sensations in the leg or foot.
- Numbness in the affected leg.
- Muscle weakness in the leg or foot.
- Pain that worsens with movement, prolonged sitting, or bending.
- Rarely, severe cases can lead to loss of bladder or bowel control, which requires immediate medical attention.
The pain is often most intense in the buttock or descending leg, sometimes described as feeling like a sharp electric shock.
Diagnosing Sciatica
Diagnosing sciatica begins with a clinical history and physical exam, including maneuvers like the straight-leg raise test to assess nerve irritation.
Imaging such as MRI or CT scans may follow to confirm the underlying structures affecting the nerve — particularly if symptoms are severe, persistent, or worsening.
What Is Spinal Decompression Therapy?
Spinal decompression therapy is a non-invasive, drug-free treatment that gently stretches the spine using a specialized traction table or device. This controlled stretching creates negative pressure within spinal discs, which can reduce pressure on nerve roots and promote the movement of oxygen, water, and nutrient-rich fluids into injured discs and nerve-related tissues.
In simple terms, decompression helps the discs “unload” pressure that is compressing nerve roots, which may be contributing to sciatica pain.
How Spinal Decompression Helps with Sciatica
1. Relieves Pressure on Nerves
By stretching the spine in a controlled way, decompression can help reduce mechanical pressure on the nerve roots that contribute to sciatic symptoms. This may relieve irritation and inflammation as the mechanical compression decreases.
2. Encourages Disc Healing
The negative pressure created in the intervertebral disc promotes improved circulation of fluids, oxygen, and nutrients — critical elements for disc and nerve health. Over time, this may support natural healing processes.
3. Reduces Pain and Improves Mobility
Many patients experience a reduction in radiating pain and improved ability to move, sit, or stand with less discomfort after multiple decompression sessions.
4. Offers a Non-Surgical Alternative
For individuals who do not want surgery or are not surgical candidates, spinal decompression provides a gentle alternative that targets the mechanical cause of nerve compression without incisions or anesthesia.
Conventional Treatment Options
Most cases of sciatica respond well to conservative care initially, including:
1. Rest and Modified Activity
Short-term rest with avoidance of activities that worsen symptoms.
2. Physical Therapy
Targeted exercises to improve posture, flexibility, and core strength to reduce nerve pressure.
3. Pain Control Therapies
Heat/ice, NSAIDs, and muscle relaxants can ease symptoms temporarily.
4. Injections
Steroid injections near nerve roots may reduce inflammation and pain for some patients.
5. Surgery (in severe or unresponsive cases)
For persistent or severe nerve compression with neurological deficit, surgical interventions like discectomy may be considered.
While these treatments often help manage sciatica, some patients seek non-surgical but more targeted approaches when conventional methods provide limited relief. One such option is spinal decompression therapy.
Typical Decompression Treatment Process
At a clinic like The Decompression Clinic, treatment generally follows several key steps:
1. Comprehensive Evaluation
A thorough evaluation — including symptom review, posture assessment, and spinal function — is done before treatment begins. Imaging results (if available) are also reviewed.
2. Customized Treatment Protocol
Every individual’s spinal condition is unique. The clinic tailors a decompression plan based on your specific nerve compression, pain pattern, and functional limitations.
3. Decompression Sessions
During therapy, you lie on a motorized decompression table or device that gently elongates the spine. This controlled movement creates space between vertebrae and reduces pressure on the affected discs and nerves.
4. Complementary Care
Decompression is often combined with corrective exercises, stretching routines, and posture education to enhance results and support lasting changes.
Who May Benefit Most from Spinal Decompression?
Sciatica sufferers who have one or more of the following features may respond well to decompression:
- Radiating leg pain or burning sensation due to nerve compression.
- Sciatica associated with herniated, bulging, or degenerated discs.
- Chronic lower back pain with nerve involvement.
- Desire to avoid invasive surgery or long-term medication use.
A thorough clinical evaluation helps determine whether decompression is suitable, as it may not be appropriate for conditions like severe osteoporosis or unstable spinal fractures.
Supporting Lifestyle Changes for Sciatica Relief
In addition to decompression therapy, persistent or recurring sciatica often responds best to lifestyle and movement improvements:
1. Improve Posture
Proper alignment of the spine during sitting, standing, and walking reduces unnecessary pressure on spinal structures.
2. Strengthen Core Muscles
A strong core supports the lower back and reduces mechanical load on nerve roots.
3. Maintain a Healthy Weight
Excess body weight increases stress on the spine, a risk factor for sciatica.
4. Regular Gentle Activity
Walking, swimming, and stretching promote circulation and reduce stiffness without aggravating nerve compression.
Conclusion
Sciatica is a painful and often frustrating condition marked by nerve irritation or compression that produces radiating pain down the leg, numbness, tingling, and muscle weakness. It stems from a variety of causes — most commonly herniated or bulging discs, spinal stenosis, and degenerative changes in the lower back.
Early intervention with conservative treatments like physical therapy, posture correction, and pain management often provides relief. However, for those who continue to experience significant symptoms, spinal decompression therapy — as practiced at specialized clinics like The Decompression Clinic — offers a non-surgical, gentle method aimed at reducing nerve pressure, improving disc health, and promoting healing from within.
Through a tailored approach combining decompression with targeted rehabilitative care and lifestyle changes, many individuals find significant pain relief, improved function, and a way to avoid more invasive surgery — making it a valuable option for managing sciatica in today’s clinical landscape.
