Chronic Back Pain: Understanding, Managing & Healing — With a Closer Look at Spinal Decompression
Back pain is one of the most common health complaints worldwide, affecting people of all ages, occupations, and lifestyles. Whether it’s a dull ache after a long day or a debilitating pain that interferes with daily life, chronic back pain can have far-reaching effects on physical wellbeing, mental health, and overall quality of life.
In this comprehensive article, we explore what chronic back pain is, what causes it, how it affects the body and mind, and a range of modern approaches — including spinal decompression therapy — that offer hope for pain relief and long-term healing.
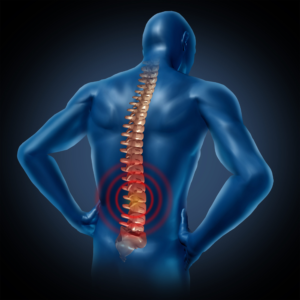
What Is Chronic Back Pain?
Back pain refers to discomfort or pain felt in the upper, middle, or lower back. When the pain persists for more than three months, it’s generally classified as chronic — as opposed to acute pain, which is short-lived and often resolves with rest or basic care. Chronic back pain can range from mild but persistent nagging to severe, constant pain that limits mobility and everyday function.
Types of Chronic Back Pain
Chronic back pain is not a single disease but a symptom that can arise from many different structural and functional problems:
01.
Mechanical pain
resulting from the movement and function of the spine, muscles, ligaments, and joints.
02.
Spinal stenosis
narrowing of the spinal canal compressing nerve roots.
03.
Discogenic or disc-related pain
arising from injured or degenerated discs between the vertebrae.
04.
Radiculopathy (nerve pain)
when spinal nerves are compressed, often leading to sciatic pain that radiates down legs.
05.
Arthritic pain
from degeneration in spinal joints (e.g., osteoarthritis).
Importantly, chronic back pain can also be non-specific — meaning no clear structural abnormality is found even after imaging. In these cases, factors like muscle imbalance, poor posture, and lifestyle habits can still perpetuate pain.
How Chronic Back Pain Affects People
Chronic back pain is more than just a physical sensation — it can affect nearly every aspect of life:
Physical Impact
Persistent pain limits mobility, stretching, bending, sitting, and standing. Simple daily tasks like tying shoes, picking up children, or commuting can become difficult. Because people tend to change movement patterns to avoid pain, this often leads to stiffness, weakness, and secondary issues in shoulders, hips, and knees.
Mental & Emotional Impact
Ongoing pain is closely linked to anxiety, depression, sleep disturbances, and decreased productivity. The brain’s pain-processing circuitry becomes sensitized, making even minor physical stress feel intense. This phenomenon, known as central sensitization, underscores the interplay between the nervous system and chronic pain. While not fully understood, research into nervous system sensitization shows how chronic pain can persist even when structural causes are less apparent.
Lifestyle Consequences
Chronic back pain reduces participation in exercise, social activities, and recreation. It can lead to weight gain, cardiovascular risk, and a lower overall quality of life.
Common Causes of Chronic Back Pain
Understanding what’s behind the pain is key to choosing the right treatments. Common causes include:
1. Herniated or Bulging Discs
Discs act as cushions between vertebrae. When they bulge or herniate, they can press on nearby nerves — triggering pain, numbness, or tingling.
2. Degenerative Disc Disease
Age-related wear and tear causes discs to lose cushioning and flexibility. This degeneration leads to inflammation and mechanical pain.
3. Sciatica & Nerve Compression
Pressure on the sciatic nerve (which runs from the lower spine down each leg) can cause sharp, shooting pain. Nerve impingement can also cause numbness or weakness in limbs.
4. Spinal Stenosis
The narrowing of spinal canal spaces compresses the spinal cord and nerve roots, leading to pain — often worsening with standing and alleviating slightly when bending forward.
5. Postural Stress & Muscle Imbalance
Poor ergonomics, long periods of sitting, and weak core muscles contribute to ongoing strain on spinal structures.
Traditional & Modern Treatment Options
There’s no one-size-fits-all treatment for chronic back pain. Instead, care is personalized based on symptoms, imaging results, and overall health.
Conservative (Non-Invasive) Treatments
Physical Therapy
Targeted exercises improve flexibility, strength, and posture.
Chiropractic Care & Manual Therapy
Adjustments and soft-tissue treatments can reduce tension.
Pain Medications
NSAIDs and muscle relaxants may offer temporary relief, though long-term use has risks.
Lifestyle Modifications
Weight management, ergonomic adjustments, and regular movement/stretches.
Interventional & Surgical Options
Injections
Epidural steroid injections sometimes help reduce inflammation.
Nerve Ablation
Targeted heat or ultrasound to disrupt pain signals.
Surgery
For certain conditions like severe herniation or stenosis not responsive to conservative care.
Spinal Decompression Therapy: What It Is & Why It Matters
One of the noteworthy non-surgical approaches to chronic back pain gaining attention is spinal decompression therapy. This is one of the core offerings at The Decompression Clinic — positioned as a specialized, non-invasive way to address pressure on spinal discs and nerves.
Understanding Spinal Decompression
Spinal decompression therapy involves gently stretching the spine to create negative pressure within the spinal disc spaces. This traction helps:
- Decrease pressure on herniated or bulging discs
- Reduce nerve compression and irritation
- Encourage inflow of oxygen, water, and nutrients into damaged discs
- Promote natural healing processes rather than just masking symptoms
In essence, decompression aims to take the load off compressed structures, giving them space and time to recover.
Non-Surgical, Drug-Free Relief
For many sufferers of chronic back pain — especially those with disc-related issues — spinal decompression offers a compelling alternative to medications and surgery. According to sources promoting decompression approaches like those at The Decompression Clinic:
- It’s non-invasive, with no incisions or anesthesia required.
- There’s minimal downtime — patients often receive treatment in clinical sessions and resume normal activity.
- The process can be integrated with other therapies such as corrective exercises and chiropractic care tailored to each individual.
Evidence & Effectiveness
While spinal decompression therapy is widely used, clinical evidence varies. Some studies suggest decompression can significantly improve pain and function in selected patients with herniated discs or chronic compression issues.
However, it’s also important to note that research findings are mixed, and not everyone responds the same way. Combining decompression with movement therapy, strengthening exercises, and lifestyle changes often yields the best outcomes.
Who Might Benefit from Spinal Decompression?
Not every back pain case is the same. Spinal decompression tends to be most effective for people experiencing:
- Chronic back pain that hasn’t responded to standard conservative treatment
- Herniated or bulging discs
- Sciatica and radicular pain
- Numbness or weakness in limbs due to nerve pressure
- Reduced mobility and flexibility due to disc compression
A comprehensive spinal assessment — including imaging and functional evaluation — helps clinicians determine if decompression therapy is appropriate.
How Spinal Decompression Works in Practice
Typically:
1. Initial Evaluation
Clinicians review medical history, posture, and imaging.
2. Personalized Plan
Based on individual needs, frequency and duration of sessions are planned.
3. Therapy Sessions
The patient lies on a motorized table. A harness gently stretches the spine, reducing pressure in the disc spaces.
4. Ongoing Monitoring
Progress is tracked, with adjustments to treatment as needed.
Sessions often last about 20–30 minutes, and a full course may involve multiple visits over several weeks, depending on severity.
Living Better with Chronic Back Pain
Chronic back pain doesn’t need to define your life. With the right combination of evidence-based treatments — from physical therapy and lifestyle adjustments to targeted interventions like spinal decompression — many people find significant relief and improved function. Whether you’re exploring non-surgical options or considering a multi-modal plan, the key is informed, personalized care that addresses both symptoms and underlying causes.
Integrating Lifestyle and Long-Term Strategies
Decompression or any clinic-based therapy is most effective when paired with lifestyle habits that support spinal health:
01.
Regular Movement
Avoid prolonged sitting; take breaks every 30–60 minutes.
02.
Strengthening Core Muscles:
Strong core muscles help stabilize the spine.
03.
Ergonomic Workstations:
Proper desk height, chair support, and monitor level can reduce strain.
04.
Mind-Body Approaches:
Practices like yoga and targeted breathing can reduce central sensitization and stress.
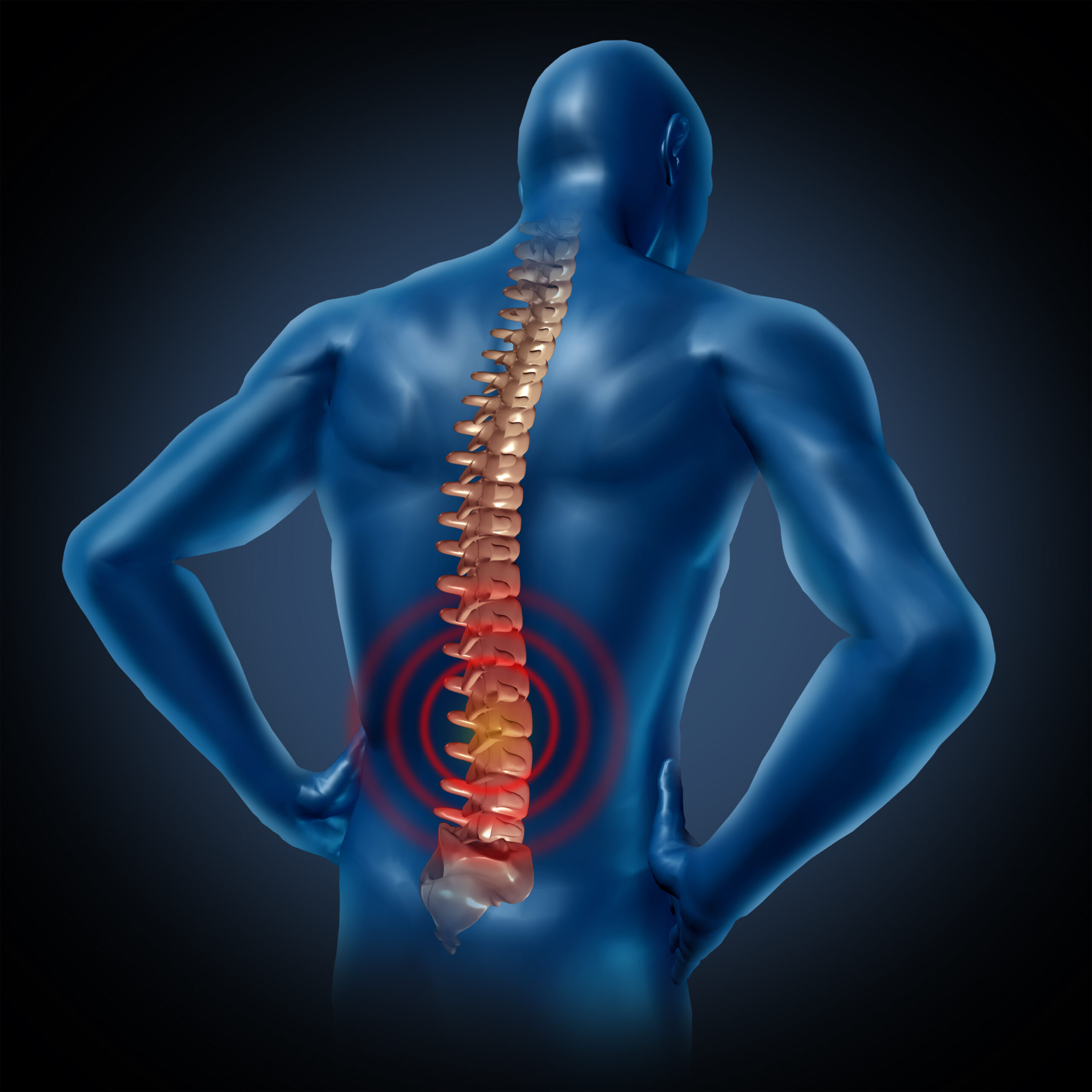
Conclusion: A Path Forward
Chronic back pain is complex and deeply personal. It can stem from structural changes, nerve compression, muscle imbalance, and even nervous system sensitization. A comprehensive understanding of your condition — and a thoughtful plan that combines medical insights with individualized care — can make all the difference.
Spinal decompression therapy, as offered by specialized clinics like The Decompression Clinic, represents one of the modern, non-invasive tools available to those seeking relief without surgery or long-term medication. But even beyond specific therapies, the real power lies in proactive care, self-management strategies, and a collaborative approach between you and your healthcare team.
With patience, perseverance, and the right support, it’s possible to move from daily pain to lasting improvement — and rediscover the freedom of a life without chronic back pain.
