Herniated Discs: Causes, Symptoms, Treatment & Relief with Spinal Decompression
A herniated disc is one of the most common and debilitating spinal conditions affecting millions of people worldwide. It can occur in the neck (cervical spine), mid-back (thoracic spine), or lower back (lumbar spine), and can range from mildly uncomfortable to intensely painful with nerve-related symptoms. Understanding the mechanics, causes, symptoms, and all available options and strategies for relief — including modern non-surgical approaches like spinal decompression therapy — empowers patients to make informed decisions about their health.
This article explains what herniated discs are, how they develop, what symptoms they cause, and how treatment options — especially non-invasive therapy at specialized clinics like The Decompression Clinic — can help patients avoid surgery and regain quality of life.
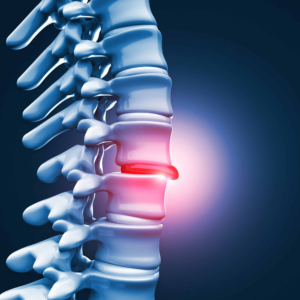
What Is a Herniated Disc?
In the human spine, vertebrae are separated by soft, cushion-like pads called intervertebral discs. Each disc has two parts:
01.
A tough outer ring called the annulus fibrosus
02.
A soft, gel-like center called the nucleus pulposus
A herniated disc occurs when the inner gel pushes or leaks through a tear or weakening in the outer ring. This is often likened to a jelly donut with a leak. When the inner material bulges outward, it can press on nearby spinal nerves, resulting in pain and neurological symptoms.
Herniated discs are also referred to as:
- Slipped discs
- Bulging discs
- Ruptured discs
- Protruding discs
They can happen anywhere along the spine, but most frequently occur in the lower back (lumbar region) and neck (cervical region).
Causes of Herniated Discs
Herniated discs arise from a combination of degenerative changes and mechanical stress. Key causes and risk factors include:
1. Age-Related Degeneration
As people age, spinal discs naturally lose hydration and elasticity. The annulus weakens, making it easier for the nucleus to bulge through even under minor stress. This process — called degenerative disc disease — explains why herniated discs are more common in people aged 30-50 and older.
2. Repetitive Strain & Poor Posture
Modern lifestyles — long periods of sitting, office work, poor posture, and repetitive lifting — place undue stress on spinal discs. Over time, this continuous strain significantly increases the risk of disc herniation.
3. Incorrect Lifting or Sudden Injury
Lifting heavy objects with your back instead of your legs or twisting while lifting increases pressure on the spine and can cause disc rupture. Similarly, falls, sports injuries, or accidents can trigger a herniation.
4. Obesity & Lifestyle Factors
Excess body weight places constant pressure on the lumbar spine. Smoking — which reduces oxygen to discs and accelerates degeneration — also raises risk. Other lifestyle factors like prolonged sedentary behavior add to cumulative wear.
5. Genetics & Connective Tissue Disorders
Some people are genetically predisposed to weaker connective tissues, which can increase susceptibility to disc problems.
These tools determine the location and severity of disc herniation and guide treatment planning.
Signs & Symptoms of a Herniated Disc
While some herniated discs cause little to no pain, many produce intense discomfort and neurological symptoms depending on location and nerve involvement. Common signs include:
Localized Pain
- Lower back pain (lumbar herniation)
- Neck pain (cervical herniation)
- Pain between the shoulder blades (thoracic herniation)
Radiating Pain (Radiculopathy)
Pressure on spinal nerves often causes pain that radiates:
- Down the buttocks, legs, and feet (sciatica)
- Into the shoulder, arm, or hand if a cervical disc is involved
Numbness & Tingling
Herniated discs can irritate or compress nerve roots, leading to numbness, tingling, or a “pins and needles” sensation in limbs.
Muscle Weakness
Compressed nerves may also weaken muscles controlled by affected nerve roots.
Symptoms with Movement
Pain often worsens during bending, lifting, or sitting, and may lessen when lying down.
Diagnosis: How a Herniated Disc Is Identified
An accurate diagnosis typically involves:
1. Medical History & Physical Exam
Doctors assess symptoms, pain patterns, neurological signs (e.g., reflexes, strength), and functional limitations.
2. Imaging Tests
- MRI (Magnetic Resonance Imaging): Gold standard for viewing soft tissues like discs.
- X-Rays: Show spine alignment and possible bone issues.
- CT Scans & EMG: Help gauge nerve involvement if needed.
Conventional Treatment Approaches
Treatment depends on the severity of symptoms, patient age, activity level, and lifestyle goals. Many cases improve with conservative care:
1. Rest & Activity Modification
Short-term rest and modifications (avoiding aggravating activities) can relieve pressure on inflamed tissues.
2. Physical Therapy
Customized exercises improve posture, strengthen supporting muscles, and ease nerve tension.
3. Medications
Over-the-counter pain relievers and anti-inflammatory drugs may reduce pain temporarily, but they don’t heal the disc.
4. Epidural Steroid Injections
These can reduce inflammation and provide temporary relief for nerve root pain.
5. Surgery (in Selected Cases)
If conservative measures fail and symptoms are severe (e.g., persistent weakness or loss of bladder/bowel control), surgical intervention like discectomy or microdiscectomy may be considered.
Most patients can return to their normal activities immediately after a session, and many experience noticeable improvement over time.
Spinal Decompression Therapy: A Key Non-Surgical Option
One of the most promising non-invasive treatments for herniated discs — and a core therapy offered at The Decompression Clinic — is spinal decompression therapy. This treatment targets the root mechanical issue rather than just masking the pain.
What Is Spinal Decompression?
Spinal decompression therapy uses a specialized machine to gently stretch the spine in a controlled manner, creating a negative pressure (vacuum effect) within the disc space. This negative pressure:
- Reduces pressure on herniated or bulging discs
- Encourages retraction of displaced disc material
- Improves nutrient and oxygen delivery to injured discs
- Reduces nerve irritation
- Enhances natural healing processes without surgery
Unlike surgical decompression, this method is non-invasive, drug-free, and gentle, making it a preferred option for many patients seeking lasting relief without the risks and downtime of surgery.
How Spinal Decompression Works
At a clinic like The Decompression Clinic, treatment typically includes:
Initial Evaluation
A comprehensive assessment including medical history, physical exam, and imaging review (if available).
Customized Treatment Protocol
A tailored plan based on your condition, severity of herniation, mobility limitations, and goals.
Treatment Sessions
Patients lie comfortably on a decompression table. The machine applies gentle traction to the spine, creating space between vertebrae. This decompresses the affected disc and reduces nerve pressure while muscles and soft tissues relax.
Integrated Therapeutic Approach
The clinic often complements decompression with chiropractic adjustments, corrective exercises, soft tissue therapies, and lifestyle guidance for long-term spinal health.
Benefits of Spinal Decompression for Herniated Discs
Many patients report significant improvements, including:
01.
Reduction in Chronic Pain
By addressing the mechanical cause of pain, decompression often provides relief where symptomatic treatments failed.
02.
Improved Mobility & Flexibility
Restoring disc height and reducing nerve pressure helps increase range of motion.
03.
Non-Surgical & Drug-Free
There’s no need for incisions, anesthesia, or long recovery time — making this ideal for patients seeking gentle, long-term solutions.
04.
Potential for Disc Healing
The vacuum effect encourages retraction of herniated material and better disc hydration — factors important for long-term disc health.
Who Might Benefit Most from Spinal Decompression?
Spinal decompression is often a good option if you:
- Have chronic back or neck pain from herniated or bulging discs
- Experience radiating pain, tingling, or weakness due to nerve compression
- Prefer a non-invasive approach
- Want to improve mobility without surgery or long-term medication
However, it may not be suitable for severe fractures, uncontrolled osteoporosis, spinal infections, tumors, or severe spinal instability — so a thorough evaluation is essential.
What to Expect: Timeline & Results
Most patients undergo multiple sessions — often 2-3 times per week over several weeks. Many begin noticing reduced pain within a few sessions, with significant improvements typically emerging by 4-8 weeks of consistent therapy.
Unlike surgery, results build gradually as the body responds to decompression and complementary therapies.
Integrating Lifestyle & Long-Term Spine Care
Spinal decompression therapy is highly effective when incorporated into a holistic plan that includes:
- Postural awareness and ergonomic improvements at work and home
- Core strengthening and flexibility exercises
- Weight management to reduce spinal load
- Regular low-impact activity like walking or swimming
Lifestyle optimization enhances decompression outcomes and helps prevent recurrence.
Patient Stories & Real Experiences
While many report excellent outcomes with spinal decompression and complementary care, individual experiences can vary. Some patients find significant pain reduction and improved function, while others find that decompression alone isn’t sufficient and require additional therapies or even surgery. The key is personalized assessment and a comprehensive approach to care.
Conclusion
A herniated disc can be a painful and life-altering condition, but it’s one for which effective treatment options exist — many of which are non-surgical, drug-free, and focused on long-term healing rather than just symptom relief.
Modern approaches like spinal decompression therapy — especially when delivered by experienced clinics like The Decompression Clinic — provide a promising path for many individuals with herniated discs. By reducing pressure on compressed discs and nerves, promoting natural healing, and enhancing spinal function, decompression offers real relief with minimal risk and downtime.
That said, the best outcomes often come from a multi-modal strategy that includes lifestyle changes, strength training, ergonomic improvements, and ongoing care. Compassionate care and informed decision-making make it possible to transition from chronic pain toward lasting spinal wellness.
