Nerve Compression: Causes, Symptoms, Treatment & Role of Spinal Decompression
What Is Nerve Compression?
“Nerve compression” (sometimes called a pinched nerve) is the result of pressure on a nerve — often from surrounding tissues such as bones, ligaments, muscles, or discs. When this pressure disrupts the nerve’s ability to transmit signals normally, it causes symptoms ranging from pain and numbness to weakness and tingling.
Nerves are part of the peripheral nervous system that relay information between the central nervous system (brain and spinal cord) and the rest of the body. When they are compressed, it interferes with these crucial signals. Common examples include sciatica in the leg, carpal tunnel syndrome in the wrist, and cervical radiculopathy in the neck.
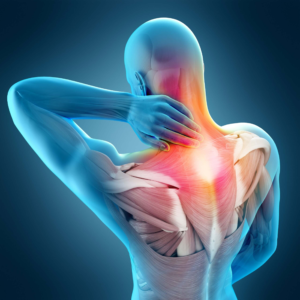
How Nerve Compression Happens
Anatomy & Vulnerability of Nerves
Nerves travel through narrow passageways in the body, often surrounded by bone, muscle, and connective tissue. Any swelling or structural change in these areas can compress nerves.
Typical Mechanisms of Compression
01.
Bone Spurs & Structural Changes:
Conditions like osteoarthritis can produce bone spurs that press on nerves.
02.
Herniated or Bulging Discs:
The discs between spinal vertebrae can bulge or rupture, pressing on nearby spinal nerve roots.
03.
Inflammation & Swelling:
Rheumatoid arthritis and soft-tissue inflammation can take up space and squeeze nerves.
04.
Repetitive Stress:
Constant repeating of a motion — like typing or bending — can inflame tissues that then compress nerves.
05.
Injury or Trauma:
Sprains, fractures, and direct impacts can lead to nerve compression.
06.
Posture and Mechanical Load:
Poor body mechanics or prolonged postures (like slouching) mechanically stress nerves over time.
- FOR ASSISTANCE
Common Types of Nerve Compression Syndromes
Although nerves can be compressed anywhere, certain conditions are particularly well-known:
Sciatica
Compression of the sciatic nerve in the lower back or buttock, causing pain down the leg.
Carpal Tunnel Syndrome
Compression of the median nerve in the wrist causing numbness, tingling, and weakness in the hand.
Cervical Radiculopathy
Compression in the neck affecting nerve roots that travel down the arm.
Cubital Tunnel Syndrome
Compression of the ulnar nerve at the elbow.
Peroneal Nerve Compression
Pressure at the knee affecting foot dorsiflexion.
These syndromes illustrate how nerve compression can occur in multiple regions and produce varying kinds of symptoms.
Types of Nerve Compression: Central vs Peripheral
The nervous system comprises the central and peripheral divisions:
Central Nerve Compression
Compression within the spinal cord itself — often due to spinal stenosis, tumors, or major trauma — can affect multiple nerve pathways and sometimes lead to serious neurological outcomes such as loss of bowel or bladder control, or limb weakness.
Peripheral Nerve Compression
Peripheral nerves exit the spinal cord to reach limbs and organs. Compression here — such as in carpal tunnel or sciatica — tends to produce local symptoms like numbness or pain in hands or feet.
Understanding this distinction is important for diagnosis and treatment direction.
Spinal Decompression Therapy: A Non-Surgical Approach
What Is Spinal Decompression?
Spinal decompression therapy is a non-surgical, drug-free treatment designed to gently stretch the spine, changing its alignment and reducing pressure on discs and nerve roots. It uses a specialized table or device that applies controlled traction to targeted regions of the back or neck.
This traction creates a negative pressure inside the spinal discs, which can help:
- Retract herniated or bulging disc material
- Reduce pressure on compressed nerve roots
- Promote circulation of oxygen, water, and nutrients, which are essential for healing.
Mechanistically, this reduces the mechanical load that leads to nerve compression in conditions related to structural spinal changes.
Symptoms of Nerve Compression
Symptoms generally occur in the area served by the compressed nerve and may include:
Pain
A sharp, burning, aching, or shooting pain near the compressed nerve.
Numbness and Tingling
A “pins and needles” sensation or loss of sensation in the affected limb.
Muscle Weakness
Loss of strength in muscles controlled by the nerve, which can affect coordination and function.
Reduced Function
Difficulty executing movements or holding objects, depending on which nerve is involved.
Symptoms Worsening with Movement
Symptoms often intensify with certain movements or positions that increase pressure on the nerve.
Diagnosing Nerve Compression
A thorough medical evaluation is critical to pinpoint who needs aggressive therapy versus conservative care. Key steps include:
A physician assesses symptoms, posture, and functional limitations.
Tests like electromyography (EMG) and nerve conduction studies measure how well nerves transmit signals.
MRI and sometimes ultrasound or X-rays help visualize nerve compression, structural causes like herniated discs, bone spurs, or cysts.
Conventional & Non-Surgical Treatments
Rest and Activity Modification
Avoiding positions or activities that exacerbate nerve pressure can significantly reduce symptoms.
Physical Therapy
Specific stretches and strengthening exercises improve flexibility, posture, and nerve gliding, which can relieve compression.
Medications
NSAIDs (e.g., ibuprofen, naproxen) and sometimes nerve-pain medications may relieve symptoms temporarily.
Steroid Injections
Targeted corticosteroids can reduce inflammation where nerves are irritated.
Splints or Braces
Used to immobilize areas like the wrist or elbow and reduce pressure on a nerve.
Surgery
When conservative treatments fail, surgical decompression aims to physically relieve the source of nerve pressure (e.g., removing a bone spur or herniated disc).
While these options form the backbone of traditional care, there’s increasing interest in non-invasive modalities that act directly on the mechanical contributors to nerve compression — and spinal decompression therapy is among them.
How Spinal Decompression Works
When you lie on a decompression table:
- Gentle Controlled Traction is applied using computerized settings that respond to your body and comfort level.
- Negative Pressure Creation inside discs encourages bulging or herniated material to retract into safer positions.
- Pressure on Nerve Roots Is Reduced, alleviating irritation and inflammation of compressed nerves.
- Improved Nutrition to Disc Tissue occurs, supporting natural regenerative processes.
This multiphase effect makes spinal decompression a compelling non-invasive alternative for individuals whose nerve compression is linked to spinal structural problems like disc issues.
Conditions Commonly Treated with Spinal Decompression
Spinal decompression is most often applied in cases such as:
1. Herniated or bulging discs
putting pressure on nerve roots
2. Sciatica
due to lumbar nerve compression
3. Degenerative disc disease
contributing to nerve irritation
4. Spinal stenosis
narrowing the space through which nerve roots travel
It’s crucial to be evaluated by a trained clinician to determine if decompression is suitable for your condition, especially since it may not be appropriate for severe instability or advanced osteoporosis.
Benefits and Considerations
Advantages
- Non-surgical and non-invasive. No anesthesia, incisions, or long recovery times.
- Targets mechanical causes of nerve compression.
- Promotes natural healing through improved circulation and reduced nerve loading.
- Often combined with rehabilitation exercises for more comprehensive recovery.
Considerations
- May require multiple sessions over weeks for optimal outcomes.
- Results vary among individuals; clinical evidence is still evolving.
- Not suitable for all forms of nerve compression or advanced structural spinal instability.
Integrating Lifestyle and Preventive Measures
Addressing nerve compression long-term often involves combining decompression with general lifestyle strategies:
Stay Active with Safe Movement
Regular physical activity maintains flexibility and improves blood flow, which supports nerve health.
Ergonomic Adjustments
Improving posture at work and during daily routines can reduce repetitive compression forces.
Weight Management
Excess body weight increases mechanical stress on spinal nerves and joints.
Strength and Stretching Exercises
Strengthening supporting muscle groups — especially the core and back — stabilizes the spine and reduces nerve stress.
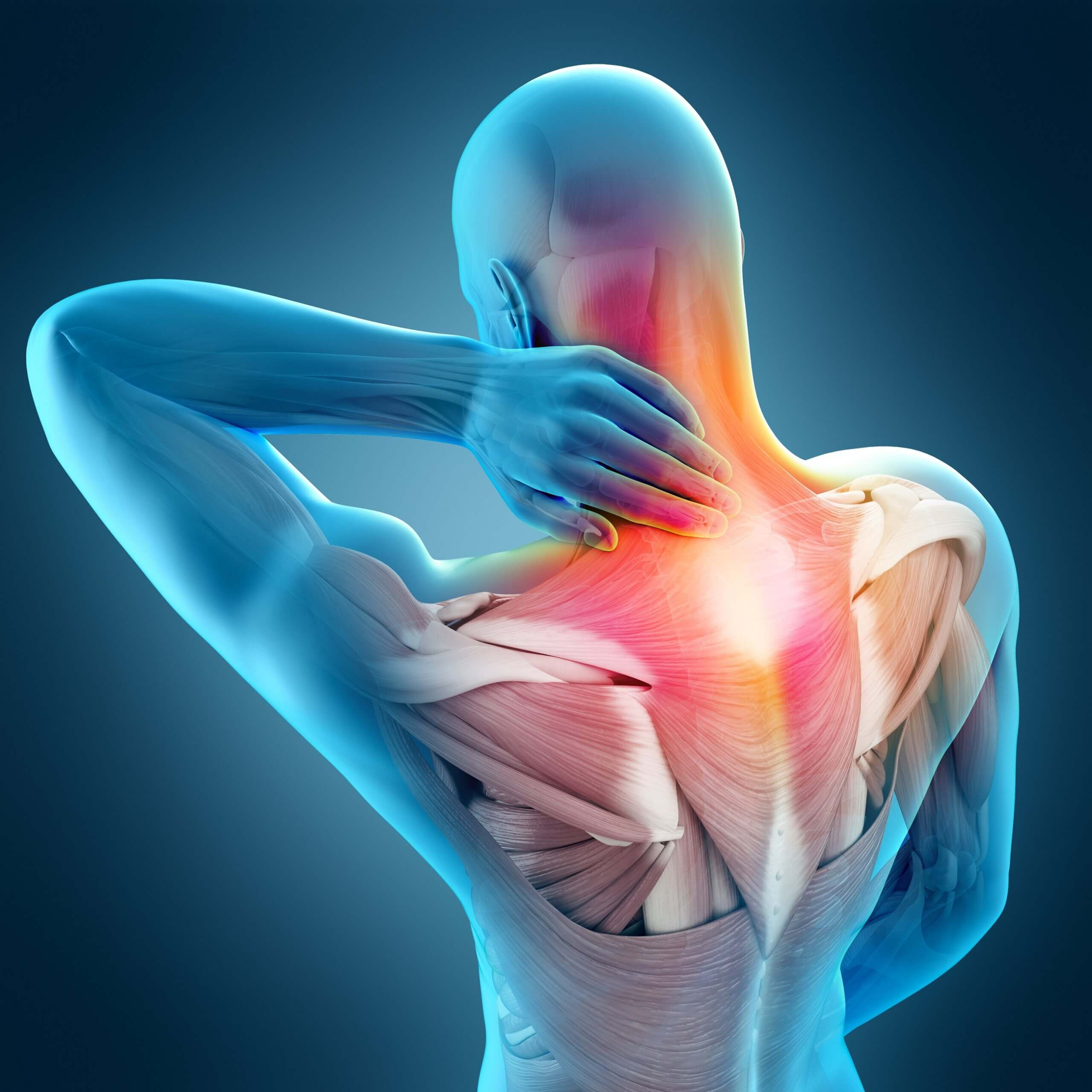
Summary
Nerve compression is a broad medical condition in which pressure from bone, muscle, ligament, or discs interferes with nerve function — and this can significantly impair sensation, movement, and quality of life. Symptoms can range from mild numbness to severe weakness, tingling, or sharp pain.
Diagnosis often involves clinical assessment, neurological testing, and imaging to accurately localize and characterize the compression. Conservative non-surgical care — such as physical therapy, medications, and activity modification — remains the first line of treatment, with surgery reserved for persistent or severe cases.
Spinal decompression therapy offers a modern, non-invasive approach that works by reducing pressure on spinal discs and nerve roots, promoting natural healing processes and relieving compression mechanically. This makes it a promising option for people whose nerve compression stems from disc-related spinal issues.
Combining clinical therapies with lifestyle and ergonomic changes provides a comprehensive strategy for managing nerve compression and improving long-term spinal and neurological health
